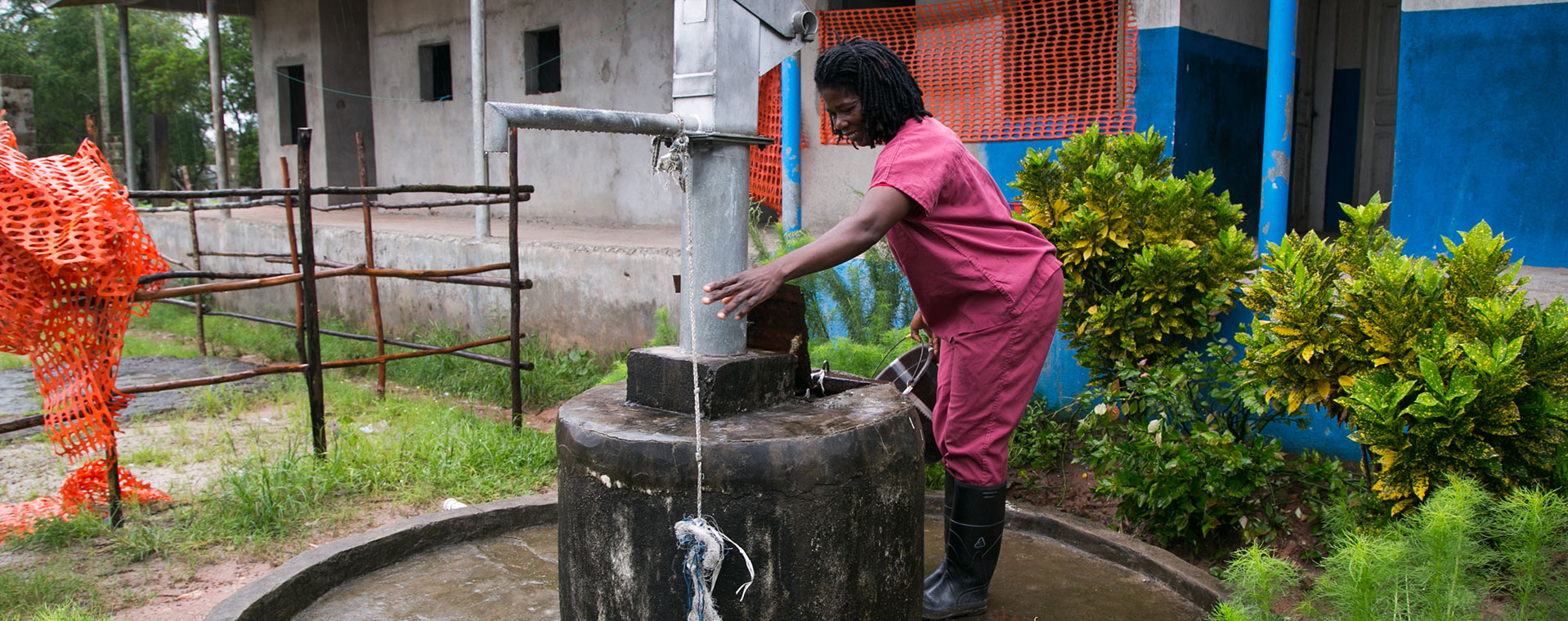Ethiopia: Village Health Partnership is Building a Model Healthcare System One Step at a Time
STORIES |

The World Health Organization and UNICEF estimate that internationally at least 1.5 billion people rely on healthcare facilities that lack proper sanitation and clean water. The situation is particularly acute in Ethiopia, one of the poorest counties in the world, with one of the world’s highest maternal and neonatal mortality rates. In rural Ethiopia 89 percent of women deliver their babies at home, 1 in 10 mothers die in childbirth, and another 1 in 2 develop a debilitating complication of childbirth.
Within Ethiopia, the West Omo Zone (WOZ), located in the nation’s rural southwest, is one of the poorest and most underserved parts of the country. In the WOZ pregnant women have little to no access to emergency obstetric care including lifesaving caesarian sections and minimal access to skilled assistance at the time of delivery. What’s more, in 2016, when we visited healthcare facilities in the zone, none had year-round access to an adequate supply of clean water, sanitation was abysmal and medical providers were not able to practice clean and safe healthcare. It was clear that healthcare facilities were actually deadly places to deliver.

In response, Village Health Partnership (VHP), Afro Ethiopia Integrated Development (AEID), Water Engineers For The Americas And Africa (WEFTA), the Mizan Tepi University Teaching Hospital (MTUTH) and Ethiopian Government and community stakeholders are working together to build a replicable system of healthcare in the WOZ.
The first step has been to create infrastructure for water, sanitation, and hygiene (WASH) and clean and safe healthcare (CASH) in eight strategically located health care facilities (two district hospitals and six health centers) close to where people live. In this effort, working with stakeholders, we are cleaning medical compounds and facilities, implementing biohazard areas with placenta pits and incinerators that allow for the safe disposal of medical waste, building concrete pit latrines, placing hand washing stations in patient care areas, and creating access to clean water by implementing borehole wells, rainwater catchment systems, gravity-fed spring catchment systems and hand-dug wells with pumps.

WASH facilitates CASH, which is the foundation of all healthcare.
The second step has been to implement infrastructure for maternal health. We aim to give pregnant women a safe place to stay when they come in seeking medical care. In the past women have had to walk great distances, even though war zones, to access care. Once they arrived at a health facility, they had no place to stay and would often have to sleep out in the rain without food and water as they waited for care. We are building fenced maternity waiting areas with kitchens, showers, and concrete pit latrines with clean water.
The third step is to train rural healthcare providers, including nurses and nurse midwives, in CASH, neonatal resuscitation, and basic emergency obstetric care. Our program teaches neonatal resuscitation using the Helping Babies Survive curriculum and critical delivery skills using the Johns Hopkins Program for International Education in Gynecology and Obstetrics (Jhpiego) Basic Emergency Maternal Obstetric and Neonatal Care curriculum. We are integrating key CASH concepts into both of these programs. We are also working with stakeholders to train technicians and create a system for maintaining what we have implemented. The goal is to ensure the ongoing practice of CASH and to maintain the healthcare infrastructure that is being implemented in the WOZ.
Finally, to ensure sustainability, we are working to connect the regional hospital in Mizan Teferi/Aman to outlying health facilities through a monitoring and evaluation program, education and training programs for healthcare providers, and a mentoring program that links facility administrators and healthcare professionals.
We have successfully implemented infrastructure for WASH and maternal health in five medical facilities. in the WOZ. This year we plan to implement WASH and infrastructure for maternal health in three more facilities. Our success is already having a ripple effect throughout the WOZ with the creation of a clean and safe health system of care. We are impacting pregnant women and neonates along with the entire community that comprises more than 500,000 people. In the future, we hope to expand our work to all 39 health care facilities in the WOZ and the neighboring Bench Sheko Zone, ultimately impacting the lives of 1.8 million people.